What is Glaucoma?
Glaucoma is one of the leading causes of blindness as people age. Ito ay mahalagang maagapan dahil ang kondisyong ito ay humahantong sa pagkabulag. Thankfully, through modern science, early detection and proper treatment, the worst can be prevented. Ibig sabihin, hindi dahil may glaucoma ay sigurado na ang pagkabulag. Pwede pa rin itong maiwasan! Know more about it.
To understand glaucoma, we must be familiar with our eyes.
The eye is made up of different parts and among these parts, our focus is the optic nerve. This is made of tiny nerve fibers kung saan para itong isang mekanismo na binubuo ng maraming maliliit na kable. These fibers are important for a person to see and when parts of them die, it causes blind spots. The affected parts of the optic nerve may have no image detection. Eventually, when all fibers of the optic nerve are dead, it leads to a black out, a total blindness. At this point, the damage caused by glaucoma is no longer treatable.
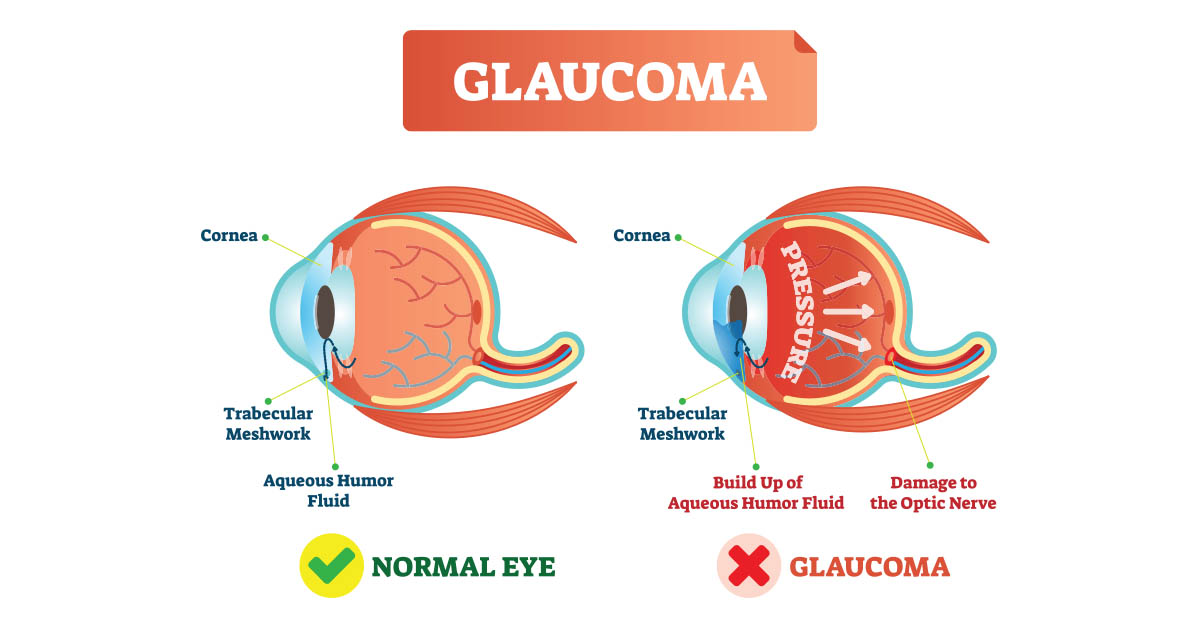
Vigilance is key because glaucoma is a silent condition that goes unnoticed until it’s too late. Initially, there is no vision change and it is painless. Its symptoms start quite slowly until it develops further, and it becomes more serious. To avoid this, the only and best option is to get a comprehensive dilated eye exam. It is easy and painless, and it helps identify signs of damage.
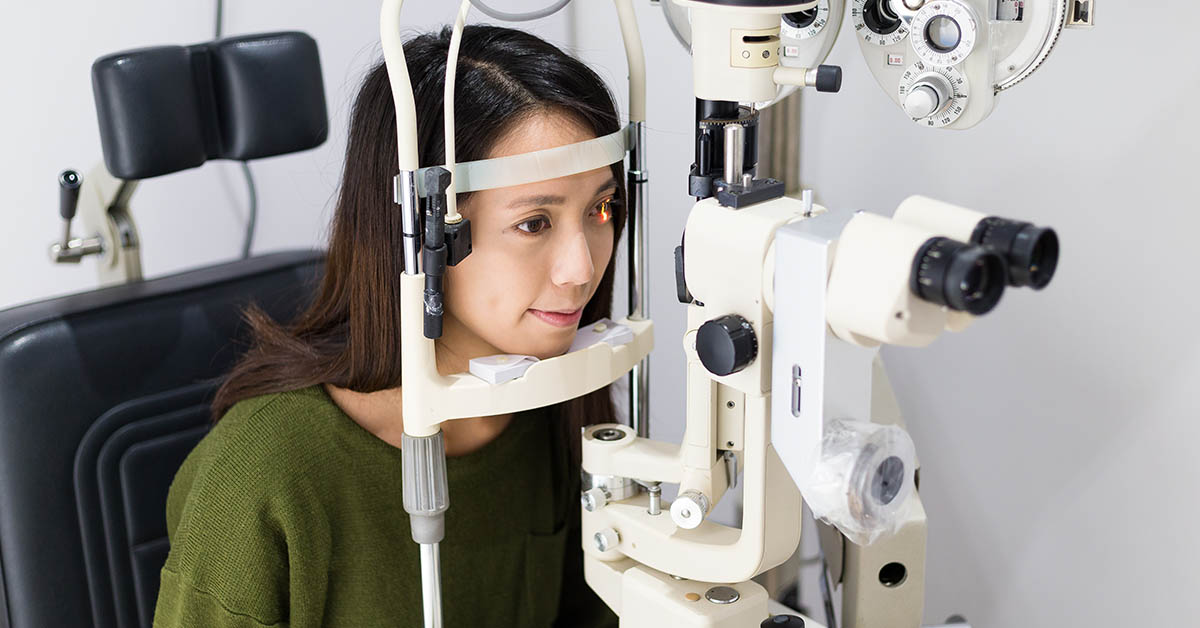
This assessment is conducted by an ophthalmologist (isang espesyalista ng mata) who will dilate the eyes with the help of some eye drops then get a magnified 3D view of the optic nerve and be able to measure the thickness of the cornea. Moreover, this is followed by a visual field test to check the patient’s peripheral vision and other tests to check for eye pressure and the eye’s drainage angle. After all of the eye exams, the final diagnosis is provided with the help of both an ophthalmologist and optometrist. The patient can then consult with a doctor and/or health care provider for options to move forward.
Who can have Glaucoma?
- People between the age of 40 to 60
- People who are sensitive to normal eye pressure
- People who have a family history of glaucoma
- People with certain health conditions like short or long sightedness, diabetes, migraines, high blood pressure, obstructive sleep apnea, and sickle cell anemia
- People who had undergone an eye operation or had an eye injury
- People who are or have been on a prolonged course of steroid medication
- People who are Hispanic, Latino, or African American
What are the Types of Glaucoma?
There are many different types of glaucoma, but the two most common types are:
The Open-angle Glaucoma. It is the most common type of glaucoma. It develops gradually when the eye’s clear fluid does not flow and drain normally. Over time, this builds pressure which causes damage to the optic nerve.
The Angle-closure Glaucoma. It is the type of glaucoma that occurs when the iris of the eye ends up blocking drainage angle. This can happen slowly or quickly but when this drainage angle gets completely blocked, eye pressure also rises. It leads to a serious eye emergency and an ophthalmologist is needed immediately to avoid going blind. This type of glaucoma must be treated right away.
Other common types of glaucoma include secondary glaucoma, that is a result of an underlying eye condition and childhood glaucoma which is a congenital and rare type of this condition that occurs in children at a very young age.
What are the Symptoms of Glaucoma?
During its early stages, it is often that there are no symptoms at all. For different types of glaucoma, the symptoms vary but in general, we have provided a list of symptoms that should be monitored.

- Having blurred vision (malabong paningin)
- Having intense eye pain (lubos na pananakit ng mga mata)
- Having a headache (pananakit ng ulo)
- Experiencing tunnel vision (paningin na makipot mula sa gitna o “fixation point”)
- Feeling of tenderness around the eyes (paglambot ng paligid ng mga mata)
- Having a red eye or red skin around the eyes (pamumula ng paligid ng mga mata)
- Experiencing upset stomach or nausea (pagsama ng sikmura o pagduduwal)
- Seeing halos or rings around lights (nakakita ng nakapalibot na pabilog na liwanag)
- Vomiting (pagsusuka)
Usually both eyes are affected although there are cases where it only happens to one eye.
How to Treat and Manage Glaucoma?
Since the complications of glaucoma after it is diagnosed are irreversible, it is important to know the options to help stop the condition from getting worse.
Medicines. Use of eye drops like the MedChoice brand of Latanoprost (LATADIN®), helps relieve eye pressure and help prevent further damage to the optic nerve. This can be used alone or with other agents. Other medications are nonspecific beta-blocker eye drops to decrease aqueous outflow.
Laser Treatment. This procedure also helps drain aqueous outflow. Since it is a simple procedure only, it can be carried out through an outpatient.
Surgery. There are different kinds of surgery that can be done to lower eye pressure. It is an option to ensure improvement of drainage of eye fluids and help prevent further damage to the optic nerve. In some cases, one surgery is not sufficient to slow down the progress of glaucoma. For these cases succeeding surgeries are required if not continued treatment through medication and rehabilitation.
Do note that diagnosing and treating glaucoma should be done right away. Other measures to manage this condition are necessary such as going through regular check-up and periodic eye exams to prevent blindness and lessen glaucoma’s impact on the patient’s daily life.
Visit MedChoice Pharma!
We hope that this article provides you with a Clear Solution, Clear Vision! Glaucoma is a foreboding disease if not treated. Remember to look out for risks and even when you do not see them, include regular eye check-ups as part of your annual activity to help diagnose and address glaucoma immediately.
Want to know more? Visit our website and learn how we ensure “Better choice. Better lives.”
References
National Eye Institute, (2022, April), Glaucoma https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/glaucoma
American Academy of Opthalmology, (2022, December), What Is Glaucoma? Symptoms, Causes, Diagnosis, Treatment https://www.aao.org/eye-health/diseases/what-is-glaucoma
Center for Disease Control and Prevention (2020, November), Don’t Let Glaucoma Steal Your Sight! https://www.cdc.gov/visionhealth/resources/features/glaucoma-awareness.html
National Health Service UK (2021, February) Overview – Glaucoma https://www.nhs.uk/conditions/glaucoma/
John Hopkins Medicine, (2023), Glaucoma https://www.hopkinsmedicine.org/health/conditions-and-diseases/glaucoma
